Hey there, fellow skin enthusiasts! We’ve all been there – one day, your skin is as smooth as silk, and the next, it’s hosting a surprise party for acne, rashes, and dry patches. If you’ve ever wondered why your skin acts like a moody teenager, the answer might lie in the hormonal changes your body goes through. Let’s spill the tea on what’s really going on beneath the surface. Riding the Hormone

1. Riding the Hormone Symphony:
Think of your hormones as the conductors of a complex orchestra. They call the shots, and your skin plays the music. When these hormones hit the high or low notes, your skin can go a little out of tune. Here’s what’s in the spotlight:
- Scabies – The Uninvited Guests: So, you thought scabies were just a random itch? Think again! Hormonal changes, like those during pregnancy, can turn your skin into a welcoming party for these tiny intruders. Cue the itchiness and redness Scabies is caused by tiny mites that burrow into the upper layer of your skin, causing intense itching, redness, and sometimes even blisters. Riding the Hormonal changes, such as those that occur during pregnancy, can make you more susceptible to scabies infestations. These uninvited guests can turn your skin into a battleground of itchiness and discomfort To combat scabies, it’s essential to consult a healthcare professional who can prescribe the appropriate treatments, such as topical creams or oral medications. Avoid scratching the affected areas to prevent further complications, and make sure to wash bedding and clothing to prevent reinfection.
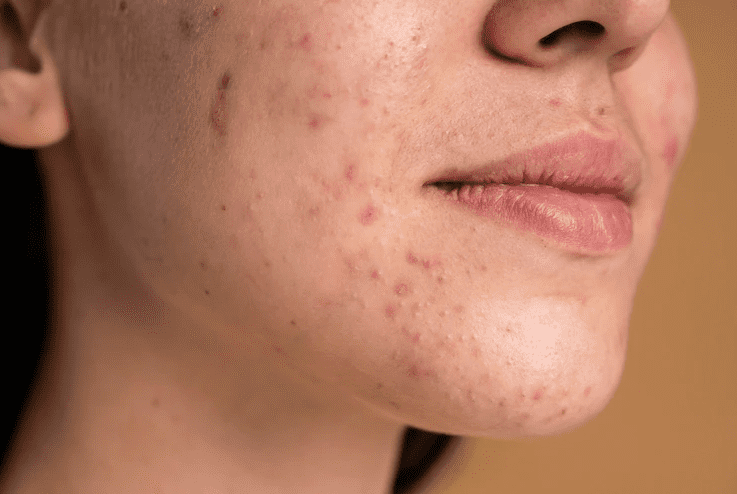
2. Melasma: Pregnancy’s “Glow” Secret
- Melasma – The Mask of Pregnancy: If you’re expecting, you might have noticed those mysterious dark patches on your face. That’s melasma, an unwelcome souvenir from hormonal changes. It’s like your skin’s way of saying, “Hey, I’ve got a surprise for you! “Melasma is often referred to as the “mask of pregnancy” because it commonly affects pregnant women. However, it can also occur in individuals who aren’t pregnant. This condition leads to the development of brown or gray-brown patches on the face, particularly on the cheeks, forehead, and upper lip. Hormonal fluctuations, especially those associated with pregnancy, can trigger the overproduction of melanin, the pigment responsible for skin color. This excess melanin results in the formation of melasma patches. While melasma isn’t harmful, it can be a cosmetic concern for many people .To manage melasma, it’s essential to use broad-spectrum sunscreen daily, wear protective clothing, and avoid excessive sun exposure. Additionally, topical treatments and procedures recommended by a dermatologist can help lighten and fade melasma patches over time.

3. The Scalp Showdown:
- Seborrheic Dermatitis – Dandruff’s Sneaky Sidekick: You know that pesky dandruff that keeps coming back? Blame it on seborrheic dermatitis, which can flare up when Hormones decide to party. Say goodbye to that little white flake on your shoulder !Seborrheic dermatitis is a common skin condition that causes redness, itchiness, and flaking, often on the scalp, but it can also affect other areas rich in oil glands, such as the face, chest, and back. While it’s typically associated with dandruff, seborrheic dermatitis can extend beyond the scalp, causing skin irritation and discomfort .Hormonal changes, stress, and other factors can exacerbate seborrheic dermatitis symptoms. The condition occurs when an overgrowth of yeast on the skin combines with excess oil production, leading to inflammation and flaking. to manage seborrheic dermatitis, consider using medicated shampoos and topical treatments prescribed by a dermatologist. These products can help reduce inflammation and control the yeast overgrowth responsible for the condition. It’s also important to maintain good skincare and haircare practices to minimize flare-ups.
4. Hormones and Sweat Glands: The Odd Couple
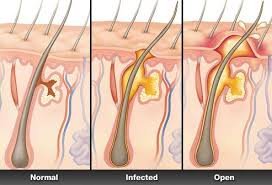
- Hidradenitis Suppurativa – When Sweat Glands Rebel: Hormones, especially in women, can stir up hidradenitis suppurativa – a painful condition that makes your sweat glands act out. Imagine your sweat glands throwing a temper tantrum – not fun! Hidradenitis suppurativa (HS) is a chronic skin condition characterized by painful, inflamed lumps that develop in areas where skin rubs together, such as the armpits, groin, buttocks, and under the breasts. These lumps can rupture and form tunnels beneath the skin, leading to abscesses and scarring .While the exact cause of HS is still not fully understood, hormonal factors are believed to play a significant role. It often starts after puberty and tends to worsen during menstruation and other hormonal changes. Excess sweat production and friction can further exacerbate the condition. Managing hidradenitis suppurativa requires a multidisciplinary approach. Dermatologists may recommend a combination of treatments, including antibiotics, anti-inflammatory medications, lifestyle modifications, and in some cases, surgical procedures. Maintaining good hygiene practices and wearing breathable clothing can also help reduce flare-ups.
5. Skin Cancer: More Than Sunscreen

- Skin Cancer – Hormones in the Mix: We often associate skin cancer with sun exposure, but hormonal changes, particularly during menopause, can increase your risk. It’s not just about sunscreen; it’s about keeping those hormones in check too! Skin cancer, including melanoma, basal cell carcinoma, and squamous cell carcinoma, is commonly linked to UV radiation from the sun and tanning beds. However, hormonal changes can also contribute to an increased risk of skin cancer .During menopause, women experience a drop in estrogen levels, which can affect the skin’s elasticity and thickness. This hormonal shift, combined with cumulative sun exposure over the years, can raise the risk of skin cancer. Additionally, some hormonal therapies, such as hormone replacement therapy (HRT), may also influence skin cancer risk. To reduce your risk of skin cancer, it’s essential to practice sun safety, including wearing sunscreen, protective clothing, and avoiding tanning beds. If you’re undergoing hormonal therapies or experiencing hormonal changes, consult your healthcare provider for regular skin examinations and advice on cancer prevention.
Conclusion:
In the grand play of life, hormones are like the backstage crew, working tirelessly to ensure everything runs smoothly. Sometimes, they create a little chaos for your skin. But fear not! Understanding the connection between hormonal changes and your skin’s quirks can help you take better care of your skin.
So, let’s embrace our skin’s unique journey through hormonal changes, give it some love, and remember that consulting a dermatologist is like having a skin’s best friend.
Keep rocking that radiant skin, you fabulous humans!

